Dr. Ashton-Miller directs the Biomechanics Research Laboratory in the Department of Mechanical Engineering at the University of Michigan. Dr. Ashton-Miller mentors several young faculty, several post-doctoral fellows, three doctoral students, several masters students and several undergraduates each semester. He collaborates closely with clinicians in a number of departments at Michigan Medicine including Dr. John O.L. DeLancey (Obstetrics & Gynecology), Neil B. Alexander (Geriatrics), James K. Richardson (Physical Medicine & Rehabilitation), Janis M.Miller (Nursing), James T. Eckner (Physical Medicine & Rehabilitation) and Edward M. Wojtys (Orthopedics). These collaborations provide students with many opportunities for interesting research projects at every level. A central focus of his research, which employs both theoretical and experimental approaches, is to develop mechanistic insights that can be used to better diagnose, treat, and even prevent selected unintentional injuries associated with life-long sequelae. This is because these sequelae cost our society billions of dollars per year in direct and indirect costs. The research falls into the following main areas:
Falls and Mobility in the Elderly and Peripheral Neuropathy (~80 publications):
In the early 1990s Dr. Ashton-Miller started working on the biomechanical risk factors for falls and fall-related injuries in the elderly. The first studies to investigate how age affects the foot clearance afforded by humans as they step over obstacles were published in 1991 & 1994. A companion 1994 paper in Gait & Posture, using the apparatus designed by Dr. Ashton-Miller, demonstrated that healthy young and elderly humans can even inadvertently trip and fall on a flat surface if they adjust their step pattern too rapidly to avoid stepping on a suddenly appearing stripe of light that they were asked to view as an obstacle if it appeared. The team also employed that set-up in a 1996 paper to perform one of the first studies demonstrating the adverse effect of multitasking on obstacle avoidance, especially in the elderly. There followed a series of articles on analyzing the effects of age on the ability to recover from a forward fall. Beginning in 2001 another series of five papers reveal how impact velocity, elbow angle, and upper arm stiffness and damping properties interact to increase the risk of wrist fracture while arresting forward falls with the arms. These studies help explain why certain falls onto the hands result in wrist fracture while others from the same height don’t. Dr. Ashton-Miller’s work was quoted in the New York Times, March 11, 2008.
His mentorship of Dr. James K. Richardson (PM&R) led to him being awarded a 5-year NIH K23 Career Development Award and more recently his first NIH R01 grant. This work has identified the biomechanical risk factors for falls, and most recently, fall-related injuries in for the first time, especially diabetic patients with peripheral neuropathy. The latter results are significant because the major socioeconomic costs are related to fall-related injuries, not falls. Doctoral students Sibylle Thies and Hogene Kim have published a series of papers on how uneven surface gait environments and the shoes with remotely controlled actuators hidden in the soles demonstrate the presence of gait deficits better than smooth surfaces.
In a series of three papers that started with the 2003 ASB Clinical Biomechanics Award, Alaa Ahmed developed a novel theory for how the central nervous system detects a loss of balance. It postulated that the brain uses an internal model of the human’s interaction with his/her environment, and compares predicted and actual accelerations to generate the error signal which the brain uses as a signal to detetct the loss of balance. This work continues with present ME doctoral candidate Payam Mirshams Shahshahani who is studying how the brain coordinates balance in a multilink 3-D dynamic model.
Vaginal Birth-Related Injuries, Incontinence & Genital Prolapse in Women (~60 publications):
Currently about 11 % of U.S. women undergo surgery for pelvic floor impairments. In the early 1990’s Dr. Ashton-Miller initiated a collaboration with Dr. John O.L. DeLancey (Obgyn) that continues to this day. This collaboration led to Dr. DeLancey being awarded his first NIH R01 grant and together with Dr. Ashton-Miller they have since received over nine national/international prizes for their work on the pathomechanics of maternal birth-related injuries and their sequelae. In September 2003 they were awarded their first 5-year National Institutes of Health Specialized Center of Research (SCOR) on “Birth-Related Pelvic Floor Dysfunction”, a Center that was competitively renewed for another five years in November, 2007, and again in October, 2012. Together they have developed the world’s only collection of standardized MR and clinical studies of pelvic floor impairments involving over 1,200 women with and without pelvic floor impairments across the age span. One of their studies (Kearney et al. 2006) demonstrated that the use of forceps increases the risk for pelvic floor injury during vaginal birth 14-fold, helping to relegate forceps to all but the most difficult births where the baby’s or mother’s life is in danger. The dogma currently is that a vaginal prolapse is caused by a failure of the tissue of the vaginal wall. Their doctoral student Luyun Chen used MR studies and computer models to contradict this dogma by demonstrating that the most likely cause of anterior wall prolapse (“fallen uterus”) is the vaginal birth stretch-related injury of the levator ani muscles. This injury impairs the muscular support of the uterus, thereby allowing intraabdominal pressure to apply a chronic pressure differential across the distal vaginal wall, thereby “pushing” that wall distally out of the body. Their postdoctoral student Jiajia Luo identified a different mechanism as the cause of posterior vaginal wall prolapse. Their goal is to develop insights that will lead to the prevention of these female conditions in the future. This work has lead to technology transfer to industry via research contracts from the Kimberly-Clark Corporation, American Medical Systems, Boston Scientific Corp, Johnson & Johnson, Proctor & Gamble, and Hologic. These companies seek our help to improve the efficacy of surgical products and feminine hygene products using insights from our 30-member Pelvic Floor Research Group (http://obgyn.med.umich.edu/research/programs-units/pfrg), the largest and first such research group in the world. A series of their invention disclosures have, and are, being converted to patents by the U-M in this space in collaboration with Drs. William Chey (Gastroenterology), Jennifer Meddings (Internal Medicine) and Sanjay Saint (Internal Medicine).
Mechanisms of Sports-Related Ankle and Knee Injuries (~30 publications):
Sports injuries at any age can result in lifelong sequelae that restrict activity later in life. Many ‘non-contact’ sports injuries are preventable, but we first need insights into the underlying causal mechanisms. Dr. Ashton-Miller mentored Dr. Edward Wojtys (Orthopedics) to his first R01 and together they examined the effect of chronic training on spine sagittal curvature in over 2,000 juvenile and adolescent athletes. More recently, they and their student Thomas Withrow developed a method for studying the factors that result in anterior cruciate ligament (ACL) injury under impulsive loading (AOSSM Research Excellence Award, 2006). ACL ruptures often lead to the initiation of osteoarthritis in the knee within seven years, no matter whether the knee is treated conservatively or surgically. This research led to Dr. Wojtys’ first NIH R01 award under which doctoral students, Youkeun Oh and David Lipps, extended the research to examine the effect of compound impulsive loading with and without axial torques on peak ACL strain. Dr. Oh won the gold medal award for this orthopedic research at the 2010 World Congress of Biomechanics. Current dogma is that ACL injuries are caused by landing a jump with excessive valgus moment. However, his team’s results have led them to reject this hypothesis by identifying internal axial tibial torque as a more potent cause of excessive ACL strain during pivot landings. Their most recent research with doctoral student David Lipps is the first to show that the human ACL is susceptible to a material fatigue failure due to the accumulation of microdamage under cyclic loading which coalesce to cause complete rupture (Lipps et al. 2013). This is a paradigm shift because the finding changes the direction of ACL injury prevention efforts toward preventing the undue accumulation of microtrauma in the ACL. In her doctoral dissertation, Ashton-Miller’s mentee Melanie Beaulieu examined the added role of restricted hip internal rotation range of motion in exacerbating ACL strain, winning the 2014 Cabaud Memorial Award from the American Orthopaedic Society for Sports Medicine. In March 2016, Drs. Wojtys and Ashton-Miller were presented with the Kappa Delta award from the Orthopedic Research Society and American Academy of Orthopedic Surgeons for their ACL research. In 2016 they were also awarded a new 5 year R01 grant to continue their research on the mechanisms underlying human ACL fatigue injuries which they are actively pursuing at the nano, micro and macroscopic scale. Their most recent paper on this topic is by Chen J.J., et al. Am J Sports Med, 2019
Concussion and Reaction Time (~6 papers)
Several papers have been published on concussion and a method for detecting short term deficits in frontal lobe function following a concussion. This involves measuring simple and recognition reaction times (US Patent 8,657,295, Feb 25, 2014). The method has been validated against a whole body protective reaction time task (Eckner et al.). We published a paper in PLoS ONE in 2011 demonstrating a sex differences in the fastest of human reaction times – those of sprinters on the starting blocks of their heats at the 2008 Beijing Olympics. It then goes on to identify a systematic bias in Omega-Swiss Timing’s method of measuring those reaction times at the Olympic Games, and supplies a suggestion for how to fix the problem. A follow-up study of the sprinter reaction times under new rules imposed at the 2012 London Olympics is complete and suggests Omega took our recommendations and this will be supplemented with data from the 2016 Rio Olympics prior to being submitted for publication shortly. Dr. Ashton-Miller is mentoring Dr. Eckner (PM&R) during his NIH K23 career development award, NIH Loan Repayment Award, and on a related R01 grant proposal.
Spine Research (~30 publications):
Ashton-Miller’s doctoral thesis and early research investigated the pathomechanics of idiopathic scoliosis, a spine deformity of unknown etiology that occurs mostly in adolescent girls. His 3-D measurements of the mechanical properties of adolescent spine motion segments remain the only such data today. Those data were used in his 3-D theoretical model of the adolescent thoracolumbar spine. It had 17 vertebral bodies, was stabilized by 144 paravertebral and trunk muscle slips under a non-linear optimal control scheme, and was used to analyze the biomechanical factors affecting whether a curve would progress during the adolescent growth spurt.
In the early 1980s he and Dr. David Spencer published two articles in Spine on the rediscovery of the Hofman ligaments in the lumbar spine. These structures, forgotten for over a century, are commonly (and incorrectly) described by orthopedic and neurosurgeons as “adhesions”, but in fact are normal anatomy. The team demonstrated that Hofman ligaments have considerable significance in the mechanics of sciatica, the intensely painful condition that can accompany a herniated lumbar disc. There followed a decade of work on the biomechanics of the lumbar and cervical spine, low back pain, neck pain, and sacro-iliac joint function.
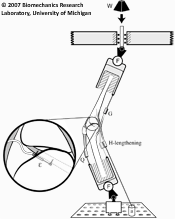
On Reducing Hand Impact Force in Forward Falls
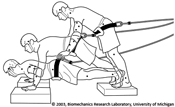
Levator Ani Muscle Stretch Induced by Simulated Vaginal Birth

Effect of Varying Hamstring Tension on Anterior Cruciate Ligament Strain During in Vitro Impulsive Knee Flexion and Compression Loading